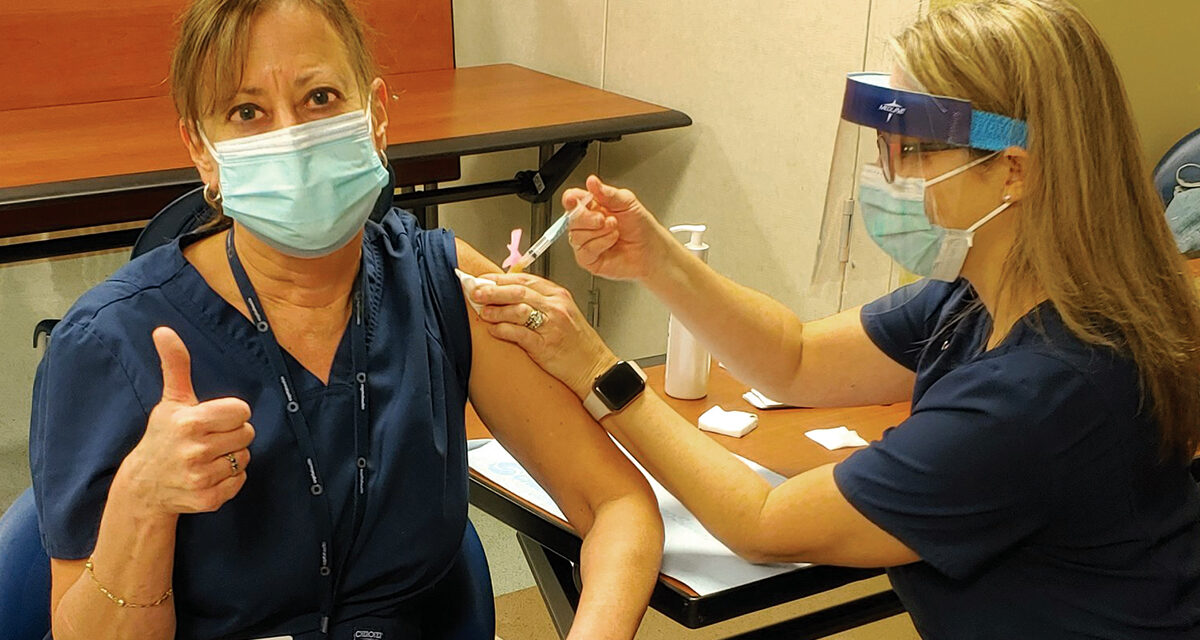
Whether you can’t wait to get your COVID-19 vaccine or are feeling hesitant to get the shot, having factual information at your fingertips will help you make an informed decision. Here’s the science-based information you need for understanding and peace of mind.
My phone buzzed with a new message notification and I saw a text from my friend Carrie. “I’m not going to get the COVID vaccine, but I want to be convinced otherwise.”
I’ve been reporting on COVID-19 and the development of the vaccines since the start of the pandemic, and my friends know I’m a staunch believer in the science behind the shots. Carrie and I have taken walks where I’ve explained to her how the vaccines’ messenger RNA (mRNA) and viral vector technology work, how the vaccine companies were able to fast-track clinical trials, and why I feel safe getting jabbed the minute it’s my turn. So when she sent me that text, I was eager to understand what was behind her hesitance.
Thirty seconds later, another ping: “I can’t get on board with the idea that these vaccines have aluminum and ethyl mercury in them. How do I rationalize that?”
I spent the next hour having a text back-and-forth with my friend, asking about her source for the ingredients information (because I knew it was wrong). In fact, there’s no aluminum or mercury in any of the COVID-19 vaccines.
Of course, Carrie is far from alone in questioning the safety of the COVID-19 vaccines. According to one online survey conducted in December 2020 by Invisibly, 47 percent of Americans are hesitant to get a COVID-19 vaccine—and of those who considered the vaccine untrustworthy, 80 percent said they were unlikely to be vaccinated. In fact, low rates of vaccine acceptance continue to be a concern around the world: New data released by the Johns Hopkins Center for Communication Programs suggests that just 63 percent of people across 23 countries will get the vaccine when it’s available—well below the 75 percent of people public health experts believe must be vaccinated to reach herd immunity.
This data points to the importance of both understanding the facts about the vaccines and also talking to friends and loved ones about them, says Rajashree Anandakrishnan, MD, a board-certified infectious disease specialist at Capital Health. “Talking about where you stand on vaccines can be taboo, but having a conversation is one of the best ways to stop the spread of misinformation,” adds Beth Battaglino, RN, CEO of HealthyWomen, a New Jersey-based organization that helps women make informed health choices.
I’m not sure I changed Carrie’s mind that day, but I learned the importance of factual information, especially when it comes to a potentially life-and-death decision like whether or not to get a COVID vaccine. The bottom line is that the science is clear: These vaccines will prevent you from getting COVID-19, and there’s nothing in them that can harm you.
No, there is no mercury in the COVID-19 vaccines
There are a lot of rumors flying around about what’s in the COVID-19 vaccines, from tracking microchips designed by Bill Gates to metals like mercury. While Facebook has committed to removing posts with false claims and conspiracy theories about the vaccines, misinformation moves fast, says Beth Battaglino, RN, CEO of HealthyWomen. “While a mercury preservative called thimerosal was used in vaccines in the past and motivated the anti-vax movement, it’s been taken out of virtually all vaccines—and it’s definitely not in these new vaccines.”
Talking about where you stand on vaccines can be taboo, but having a conversation is one of the best ways to stop the spread of misinformation.

Word of Mouth
Want to have a conversation with a friend who’s anxious, skeptical, or just plain misinformed about the COVID-19 vaccine? Follow this advice.
Get a sense of how open someone is to a discussion. No matter how top-of-mind this is for you, the danger of becoming evangelical about COVID vaccination is that your knowledge will fall on deaf ears. “You can throw out a softball by asking a friend or loved one if she has been able to schedule her vaccine, or get on a list,” says Battaglino. “It’s an open-ended, non-threatening question that’ll tell you a lot about where someone stands and how open they are to a conversation if they have any concerns.”
Avoid launching too much info at her. Science-based facts are great. But it’s also important to remember that many people who are hesitant about vaccines are just afraid, says Nadine Gartner, founder of Boost Oregon, a nonprofit dedicated to grassroots education about vaccines. “Fear is a feeling, and you can’t answer a feeling with facts. You have to answer a feeling with a feeling.” If you want to throw out one piece of factual information that might actually stick, Battaglino suggests this one: By getting the COVID vaccines, you’re protecting not just yourself, but also your kids, parents, friends, and your community.
Stay open-minded—and compassionate. When you’re fired up about a topic, it can be challenging to stay calm, cool, and collected—but it’s so important that you do, says Gartner. “If the person you’re speaking to is getting heated and throwing anti-vaccine tropes at you, understand that that’s their truth.” Then, see if they’ll also stay open to your evidence-based information—and remember to lead with love and compassion, not just the facts.
Pregnant or trying to conceive?
You can (and should!) get your COVID-19 vaccine.
The CDC, American College of Obstetricians and Gynecologists (ACOG), and doctors around the world are all on the same page on this topic: Pregnant and breastfeeding women can and should get vaccinated, says Battaglino. “I can understand women’s fears—but the research shows it’s safe,” she says.

1. How does the vaccine work?
Like all vaccines, the COVID-19 vaccine is designed to provoke an immune response so your body is able to fight the real virus if you’re exposed, says Battaglino. The first two COVID-19 vaccines approved for use—from Pfizer and Moderna—use messenger RNA (mRNA) technology, which gives instructions for our cells to make a harmless piece of what’s called the “spike protein” that’s found on the surface of the novel coronavirus. Then, the important immune system response takes place, recognizing that spike protein as a foreign invader and making antibodies that’ll protect you against COVID-19 going forward. It’s important to note that mRNA vaccines don’t use actual live coronavirus particles, which means it’s impossible to get COVID-19 from an mRNA vaccine, says Dr. Anandakrishnan.
The other two vaccines—Johnson & Johnson and AstraZeneca—use viral vectors instead of mRNA but work in a similar way, adds Dr. Anandakrishnan: Instead of mRNA, they use a modified version of a harmless virus to deliver instructions to our cells to produce the spike protein, which prompts the immune system to create antibodies.
This will help you keep the info about the current vaccines straight:
2. How can I trust a vaccine that was created so quickly via “Operation Warp Speed”?
Before the COVID-19 vaccines, the fastest vaccine developed was for mumps—and it took four years. While that might raise questions about the COVID-19 vaccine development process, there’s a logical explanation, says Erika Beard-Irvine, MD, a pediatrician in Portland, Ore. “For starters, funding and approvals for research were fast-tracked—and that’s a process that can typically take years,” she says. What’s more, researchers didn’t wait for each phase of their research trials to finish before starting the next. “By combining phases, the vaccine companies were able to test vaccines on more people without as much waiting as usual,” adds Dr. Beard-Irvine.
It’s important to note that combining phases of human trials has been done before, adds Anne Rimoin, PhD, a professor of epidemiology at the UCLA Fielding School of Public Health and Infectious Disease Division of the Geffen School of Medicine and the director of the Center for Global and Immigrant Health. “We did this when developing cancer drugs, as well as the Ebola vaccine.” Also, the research that leads to any vaccine’s approval has to be vetted by the Food and Drug Administration (FDA), “and the FDA has a very strict set of policies in place,” says Rimoin. For perspective: Less than 10 percent of drugs that enter clinical trials are ever approved by the FDA.
Another really important piece to the fast-paced development of the COVID-19 vaccines is that the “new” mRNA technology the Pfizer and Moderna vaccines use was actually founded a decade ago. To make the new vaccines, all the researchers needed to know was the genetic sequence of the protein they wanted our bodies to create, says Dr. Anandakrishnan.
3. Once I’m vaccinated, can I go back to living life like I did before the pandemic?
No, at least not yet. Being fully vaccinated doesn’t mean you can stop following public health and safety guidelines, like wearing a mask, washing your hands frequently, and social distancing. That’s because the jury’s still out regarding whether or not you can still transmit COVID-19 to others after you’ve been vaccinated, says Jeffrey Stalnaker, MD, an internal medicine specialist in Florida. While most vaccines stop a contagious virus from taking hold by prompting surface antibodies to live in our eyes, nose, and mouth that destroy virus particles before they’re able to invade the body, scientists don’t yet know if the COVID-19 vaccines mount this kind of response. They’re hopeful, but “studies are still taking place that will help us understand whether the vaccines have an impact on transmission,” says Stalnaker.
4. Why do I need the vaccine if I’ve already had COVID-19?
Experts aren’t sure if the hard-won natural immunity to the virus you have after you’ve recovered will last, says Battaglino. “Usually, the immune system remembers an infection you had so it’s better able to fight it off if you come in contact with it again,” she says. “But since the novel coronavirus is new, scientists don’t yet know exactly how long that natural immunity might stick around.” And because the vaccine has been shown to boost protection while causing very few if any side effects—even in those who’ve had COVID-19—the CDC recommends it.
5. Is someone monitoring how the vaccine rollout is going?
There are a number of surveillance systems in place—not only for the COVID-19 vaccines but for every vaccine—that are designed to catch rare side effects and provide a continual safety assessment of all vaccines. One of the biggest monitoring systems is the Vaccine Adverse Event Reporting System (VAERS), which collects reports from healthcare practitioners, vaccine manufacturers, and the public of adverse events that happen after vaccinations. Another is the Vaccine Safety Datalink (VSD), which is a network of nine health care organizations across the country that conduct active surveillance and research.
To add an additional layer of safety monitoring for the new COVID-19 vaccines, the CDC created V-safe, a smartphone-based health checker that uses text messages and web surveys to check in with people following their shots. It also provides follow-up calls to anyone who reports a serious adverse event after being vaccinated.
6. Will the vaccines protect against the new variants we keep hearing about?
We don’t know, says Battaglino. “Similar to what we see with the flu virus, we’re going to continue to see new strains of the novel coronavirus,” she says. “And just like the flu vaccine is changed every year to account for the new strains, the same may happen with the COVID-19 vaccines.” Still, what we know for sure right now is that the current vaccines are the best mechanisms we have for getting our lives and the economy back on track, adds Battaglino. “The good news is that the best scientists are studying this right now—not politicians or other elected officials, but people who’ve spent their careers studying infectious diseases,” she says. “As we continue to see new strains of the novel coronavirus, I’m confident that the science will keep up.”